Insurance and Benefit Verification

Insurance and Benefit Verification
Insurance companies don’t make it easy to verify coverage and benefits with their difficult-to-navigate systems and inconsistent data. This leads to your staff dealing with high payor call volume or inaccurate determinations.
Preyfox can remove that burden from your team allowing them to focus on patient experience instead of paperwork and ensure claim submission is not delayed.
Insurance verification and benefit determination services available include:
- Confirm insurance coverage, including dual eligibility, TP eligibility, and Out-of-State verification.
- Determine in- and out-of-network benefits and patient liability.
- Support the “No Surprises Act” billing estimate requirements for out-of-network and uninsured individuals.
WHAT TO EXPECT...
- Our Billing Specialists act as intermediaries, providing detailed status updates and weekly reports.
- Account payments are managed, collected, and posted. Additionally, our team submits claims to payers, and follows up with the insurance companies regularly to ensure the quickest possible turnaround time on payments.
- Account information is routinely reviewed to spot trends and opportunities to optimize the revenue cycle processes. Unresolved AR, claim denials, and coding issues are examined for root-cause and forwarded to the client for resolution.
The Billing Specialists responsibilities include.
- Collecting, posting and managing account payments, submitting claims and following up with insurance companies.
- Review account information to identify trends and opportunities to improve the revenue cycle process
- Research unresolved and old AR, claim denials, and coding issues (traditionally issues such as these are forwarded to the client to resolve)
- Act as client liaison, provide status updates and detailed reporting on a weekly basis
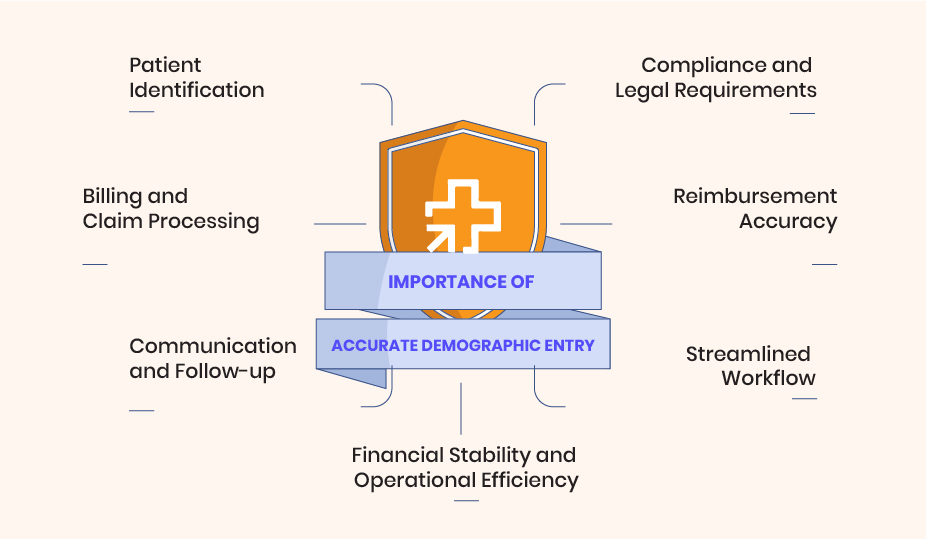
This would include Patient’s Name, Present Address, City, State, Zip Code, Social Security Number, Employer Details, Insurance Details like Primary, Secondary and Tertiary, and guarantor information.
This would include entering details like Date of Service, Referring Physician, Ordering Physician, Place of Service, Type of Service, CPT Codes, ICD Codes, Modifiers, Authorization or Referral Details and Co-pay Details.
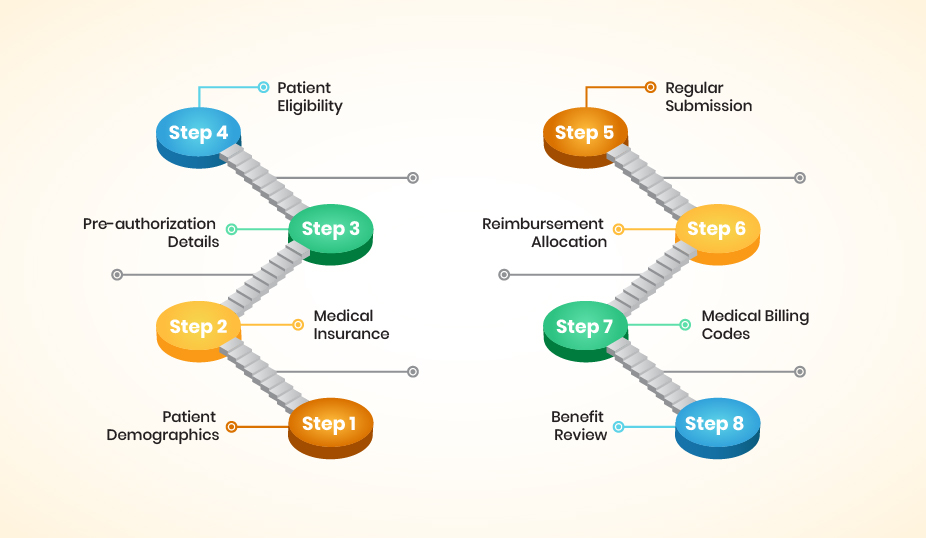
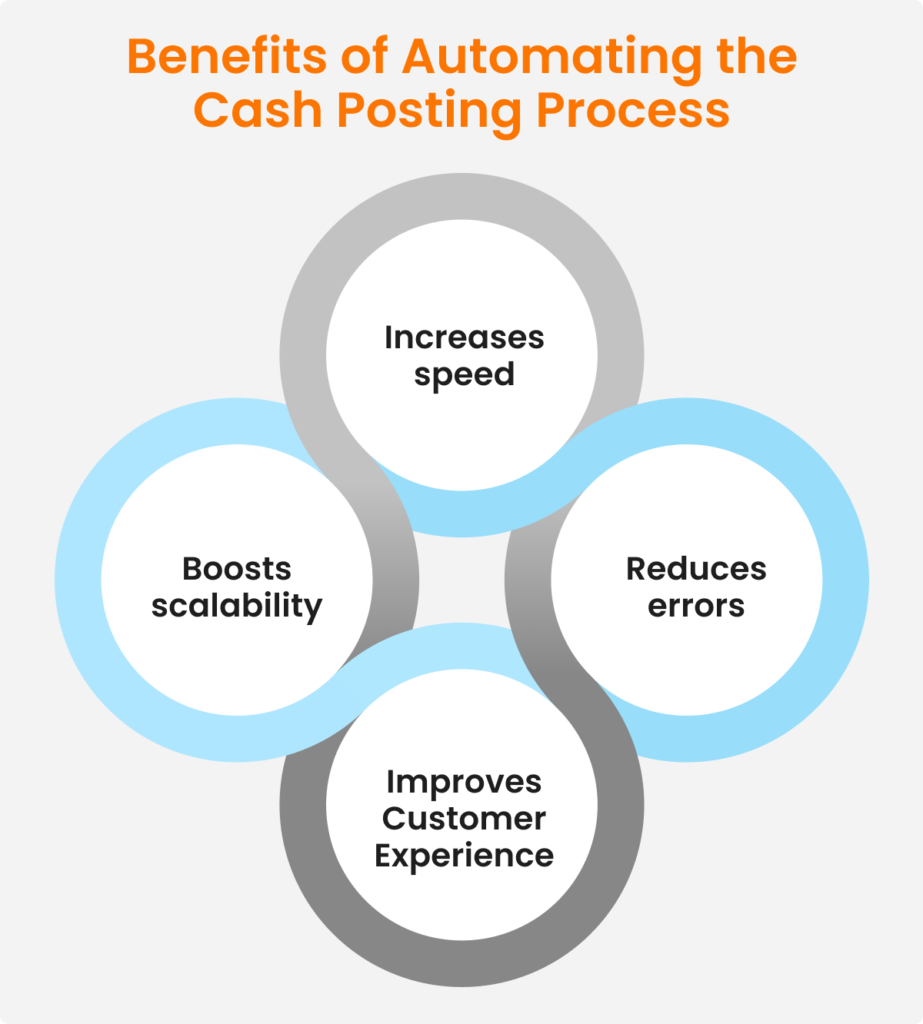
Application Cash posting is the of payments in the medical software. Cash postings are done on the basis of Explanation of Benefits (EOBs) from the respective insurance companies and the cheques sent by the patient.

